IPS Hodgkin Lymphoma Calculator: Fast Prognostic Support for Advanced cHL
Synthesize seven prognostic variables in seconds to estimate 5‑year freedom from progression and guide clinical decision-making in advanced classic Hodgkin lymphoma.
-image.webp)
Quick Navigation
Advanced classic Hodgkin lymphoma (cHL) remains highly curable, but outcomes vary widely depending on a patient’s baseline risk profile. In busy clinics, MDTs, and academic centers, synthesizing multiple prognostic variables at the point of care can be challenging—especially when decisions about regimen intensity, consolidation, or trial eligibility hinge on an accurate risk assessment.
The International Prognostic Score (IPS) for Hodgkin lymphoma is one of the most widely used tools to estimate 5‑year freedom from progression and overall survival in patients with advanced-stage disease, and it continues to inform contemporary practice and research. At OncoToolkit, we’ve built an IPS (Hodgkin Lymphoma) calculator that turns the original seven-factor score into a clean, mobile-ready interface so you can obtain an interpretable risk estimate in seconds during ward rounds, clinics, or teaching sessions. [1], [2], [3], [4], [5]
1. Understanding the IPS (Hodgkin Lymphoma) Score
The International Prognostic Score (Hasenclever index) is a seven-factor clinical score derived from a large pooled cohort of adults with newly diagnosed advanced-stage (Ann Arbor stage III–IV) Hodgkin lymphoma treated with combination chemotherapy between the early 1980s and early 1990s. It predicts the probability of 5‑year freedom from progression (FFP) and also correlates with overall survival (OS), helping clinicians stratify patients into risk groups ranging from relatively favorable to high risk. [6], [5], [1]
Each of the following adverse factors contributes 1 point to the IPS when present:
- Age >= 45 years
- Male sex
- Ann Arbor stage IV
- Hemoglobin < 10.5 g/dL
- Serum albumin < 4.0 g/dL (40 g/L)
- White blood cell count >= 15,000/mm³
- Lymphocyte count < 600/mm³ or < 8% of the white count.
The total score ranges from 0 to 7, with higher scores associated with lower 5‑year FFP and OS. Historically, the IPS was developed using multivariable Cox proportional hazards modeling and then simplified into this additive point system, making it intuitive for day-to-day clinical use. [3], [5], [1], [6]
2. Importance of IPS Risk Stratification in Practice
The IPS remains a key benchmark for risk stratification in advanced cHL and is frequently referenced in clinical trials, retrospective series, and guideline discussions. Patients with a low IPS (0–1) have historically had 5‑year FFP rates above 75–80%, whereas those with higher scores (>= 4–5) have rates closer to 40–50%, underscoring the heterogeneity within “advanced-stage” disease. This gradation can influence the perceived need for treatment intensification, consideration of novel agents, or early transplant strategies in select cases, especially in research or high-risk management pathways. [5], [7], [3], [6]
Clinical Pearl: While manual calculation at the bedside is error-prone due to the seven specific thresholds, digital tools reduce the cognitive load and "calculator fatigue," ensuring that evidence-based risk stratification is consistently applied during high-stakes MDT discussions. [4], [8], [9], [10], [6]
3. Clinical Evidence and Validation of the IPS
3.1 Statistical Methodology of the Hasenclever Index
The original IPS was derived from a multivariate Cox proportional hazards model built on data from 4,695 patients enrolled in 25 cooperative group studies and institutional cohorts of advanced Hodgkin disease. Seven variables showed similar independent adverse prognostic effects on 5‑year FFP and OS, and each was assigned 1 point to create a simple additive index. [1], [3], [6], [5]
In the original cohort, 5‑year FFP ranged from approximately 84% for patients with an IPS of 0 to about 42% for scores >= 5. Subsequent validation and contemporary series have confirmed that the IPS retains prognostic value, although outcome curves have compressed with modern regimens. [11], [7], [12], [3], [6], [5]
3.2 Key Strengths and Clinical Limitations
Major strengths include the IPS’s derivation from a large, international dataset and its reliance on routinely available clinical and laboratory parameters. It remains the most widely used prognostic index for advanced-stage cHL. [13], [3], [6], [5], [1]
Limitations to consider:
4. How to Use the IPS (Hodgkin Lymphoma) Calculator
The interface mirrors how clinicians think: each of the seven IPS variables is presented as a simple, clearly labeled question with binary “Yes/No” options. [2], [4], [1]
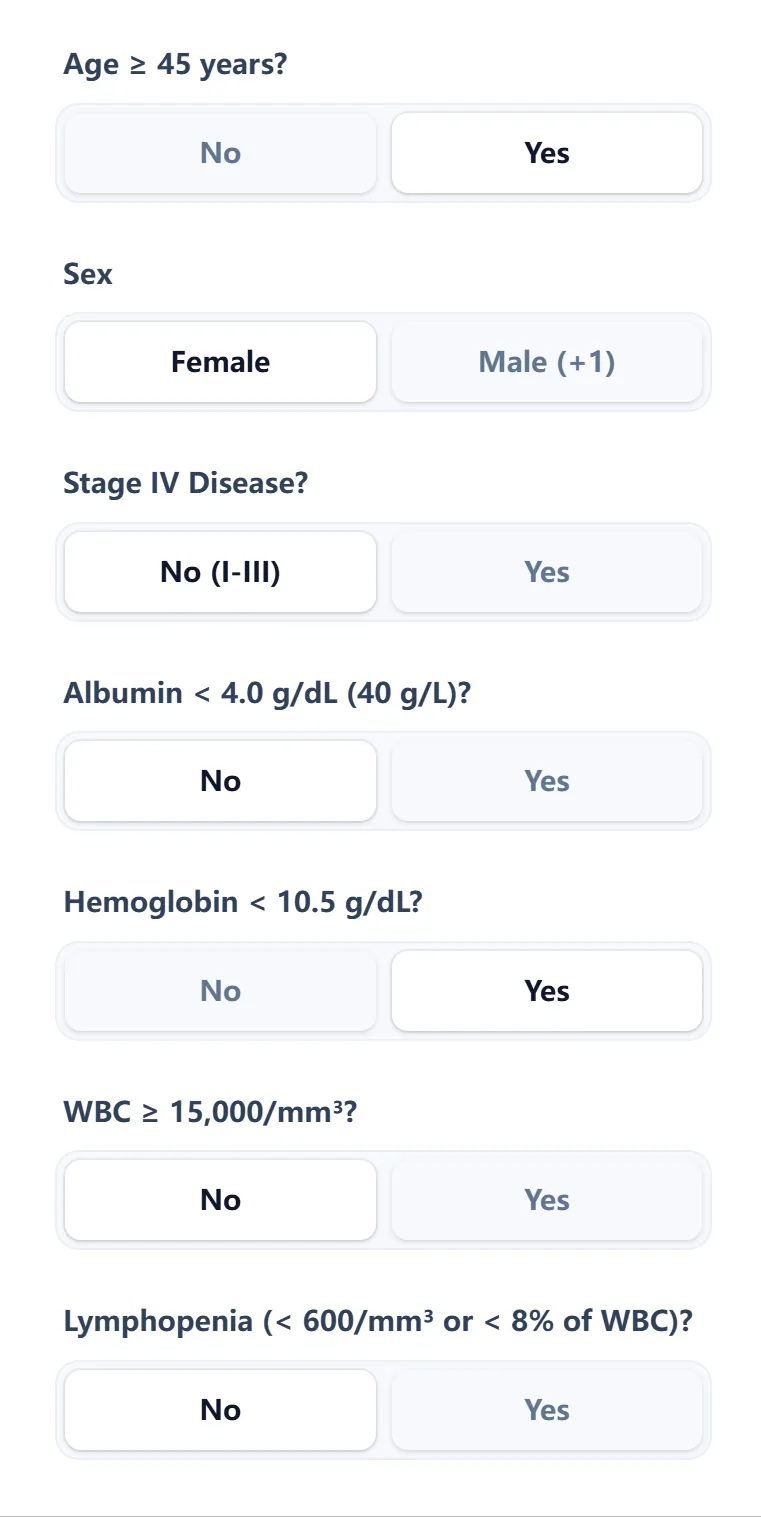
Figure 1. The IPS calculator input screen captures all seven Hasenclever risk factors using intuitive toggle buttons.
Once you select the responses, the calculator automatically sums the factors to generate the IPS (0–7). The tool maps this to a corresponding 5‑year FFP estimate and visually places the patient along a color-coded risk continuum. [3], [4], [6], [7], [1]

Figure 2. Embedded reference data links each IPS total score to the corresponding 5‑year FFP percentage.
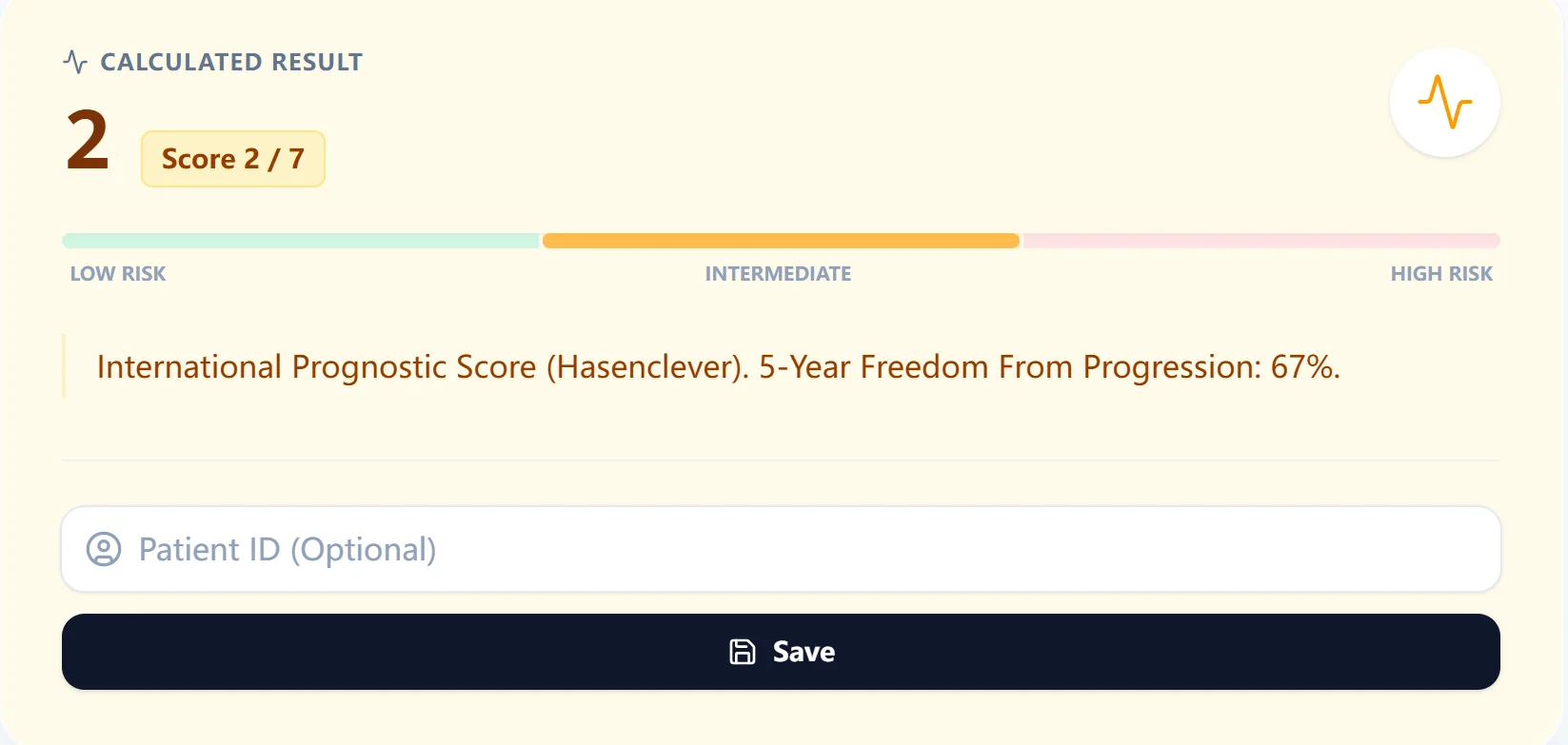
Figure 3. The result view displays the IPS, risk band, and 5‑year progression‑free estimate.
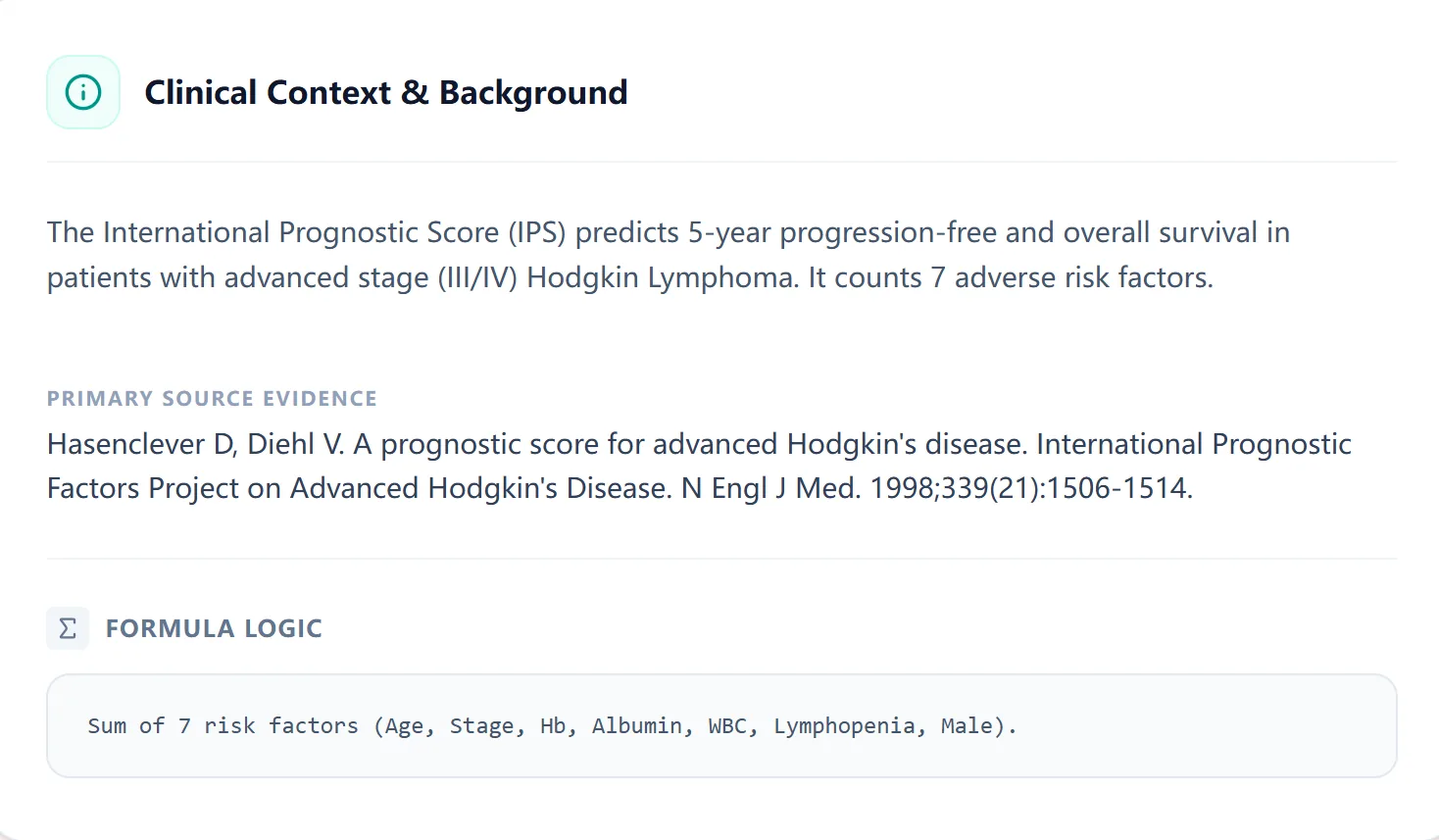
Figure 4. The clinical background section provides context on the derivation cohort and seven adverse factors.
5. Clinical Applications: Support for Care, Education, and Research
5.1 Decision Support in Daily Rounds
In day-to-day practice, you can use the IPS calculator to:
- Document baseline risk at diagnosis for stage III–IV cHL. [1], [3], [5]
- Prepare for MDT meetings by highlighting high IPS scores for deeper discussion. [3], [5]
- Inform conversations about therapy intensity or clinical trial referral. [11], [5], [3]
5.2 Medical Education and Case Simulation
For trainees, the calculator doubles as a teaching module. Supervisors can walk through hypothetical cases to show how risk changes when individual factors are toggled, reinforcing the link between disease biology (e.g., low albumin) and patient outcomes. [6], [1], [3]
5.3 Research and Quality Improvement Initiatives
Standardized tools promote consistency across institutional databases. Clinicians can monitor whether high-IPS patients receive timely referrals for advanced therapies or participate in clinical trials. [13], [3], [1], [5]
6. Clinical FAQ for the IPS (Hodgkin Lymphoma) Score
Can the IPS be used in early-stage Hodgkin lymphoma?
No. It was derived exclusively from advanced-stage (III–IV) patients. For early-stage disease, other frameworks and response-adapted PET assessments are standard. [7], [5], [1], [3]
References
- Hasenclever D, Diehl V. A prognostic score for advanced Hodgkin's disease. N Engl J Med. 1998. Source
- Medscape. Hodgkin's Disease Prognosis (IPS). Source
- Montalbán C, et al. The International Prognostic Score revisited. Blood. 2016. Source
- MDApp. Hasenclever IPS Calculator. Source
- Moccia AA, et al. International Prognostic Score in Advanced-Stage Hodgkin's Lymphoma. JCO. 2012. Source
- The Hematologist. International Prognostic Score for Advanced Hodgkin Lymphoma. Source
- Rambam Maimonides Med J. Prognostic Factors in Hodgkin Lymphoma. Source
- PMCID PMC6563614. Clinical Decision Support Tools. Source
- PMCID PMC7973455. Reducing Cognitive Load in Oncology. Source
- PMCID PMC6732014. User-Centered Design for Clinical Calculators. Source
- MedNexus. Evaluation of IPS-7 and IPS-3. Source
- Academia.edu. Evaluation of IPS in the Modern Era. Source
- Blood. International Prognostic Score for Hodgkin Lymphoma Validation. Source
Ready to Stratify Risk for Advanced cHL?
Access the IPS calculator for fast, reliable prognostic support at the point of care.
Try the IPS Calculator Now
Free to use. No registration required.