IMDC (Heng) Risk Score Calculator for Metastatic RCC
A comprehensive guide to using the IMDC (Heng) Risk Score to stratify metastatic Renal Cell Carcinoma and guide clinical decision-making.

Quick Navigation
- 1. Introduction to the IMDC (Heng) Risk Score
- 2. What is the IMDC (Heng) Risk Score?
- 3. Clinical Importance of IMDC Scoring in Practice
- 4. Clinical Evidence and Model Validation
- 5. How to Use the OncoToolkit IMDC Calculator
- 6. Interpreting Risk Groups and Survival Benchmarks
- 7. OncoToolkit: Supporting Education and Research
- 8. Clinical FAQ on IMDC Risk Stratification
1. Introduction to the IMDC (Heng) Risk Score
For metastatic renal cell carcinoma (mRCC), selecting the right first‑line and subsequent systemic therapies depends heavily on accurate prognostic risk stratification. At OncoToolkit, we’ve built an IMDC (Heng) Risk Score calculator that transforms six routine clinical and laboratory parameters into a clearly labeled risk category with historical survival benchmarks, helping oncologists and nephrologists reduce cognitive load while maintaining guideline‑aligned care. [1], [2], [3]
The IMDC (Heng) Risk Score is now the most widely used clinical model for stratifying survival in mRCC and is incorporated into contemporary treatment algorithms and clinical trials worldwide. On our platform, this calculator is optimized for quick use during ward rounds, MDT meetings, and virtual tumor boards, minimizing “calculator fatigue” so clinicians can focus on nuanced discussions about treatment goals, comorbidities, and patient preferences. [2], [4], [5], [1]
2. What is the IMDC (Heng) Risk Score?
The International Metastatic Renal Cell Carcinoma Database Consortium (IMDC) or Heng Risk Score is a point‑based prognostic model that predicts overall survival in patients with mRCC treated with systemic therapy, initially VEGF‑targeted agents. It refines the earlier MSKCC (Motzer) model by adding inflammatory markers, improving prognostic discrimination in the targeted‑therapy and immuno‑oncology era. [3], [6], [7], [8]
The score allocates one point for each of six adverse baseline factors:
- Karnofsky performance status (KPS) < 80%
- Time from diagnosis to systemic therapy < 1 year
- Hemoglobin < lower limit of normal (LLN)
- Corrected calcium > upper limit of normal (ULN)
- Neutrophils > ULN
- Platelets > ULN
The total number of risk factors (0–6) determines the IMDC group: favorable risk (0), intermediate risk (1–2), or poor risk (≥3), each associated with distinct historical median overall survival. [4], [1], [3]
3. Clinical Importance of IMDC Scoring in Practice
The IMDC risk category is tightly linked to systemic treatment selection and prognosis in metastatic clear‑cell RCC, informing decisions between dual immunotherapy, IO/TKI combinations, and VEGF‑TKI monotherapy. Many international guidelines and pivotal trials stratify outcomes and recommendations by IMDC risk group, making consistent scoring essential for evidence‑based regimen choice and patient counseling. [7], [9], [2]
From a patient‑facing perspective, IMDC groups provide a structured way to frame survival expectations while avoiding over‑precision, supporting shared decision making around therapy intensity, toxicity trade‑offs, and palliative care planning. For multidisciplinary teams—including nephrologists managing CKD or dialysis, surgeons, and radiation oncologists—the score offers a common language that anchors discussions about cytoreductive nephrectomy, local control strategies, and sequencing of systemic agents. [9], [10], [2], [7]
4. Clinical Evidence and Model Validation
4.1 The Mathematics of the Heng Model
The Heng model was derived using multivariable Cox proportional hazards regression in a large, multicenter dataset of mRCC patients treated with VEGF‑targeted therapies, identifying six independent predictors of overall survival. Because the hazard ratios for these predictors were of similar magnitude, they were simplified into an unweighted point system in which each adverse factor contributes one point to the total score. [6], [3], [7]
4.2 Validation Across Global Cohorts and Modern Therapies
The IMDC score has been externally validated in multiple international cohorts involving thousands of patients, consistently demonstrating separation in overall survival among favorable, intermediate, and poor risk groups. Subsequent studies have confirmed that IMDC categories retain prognostic significance in patients receiving immune checkpoint inhibitors, combination IO/TKI regimens, and non–clear‑cell RCC subtypes. [10], [13], [4], [7]
4.3 Clinical Limitations and Thoughtful Application
As with any prognostic model, the IMDC score provides group‑level estimates and should not be interpreted as a precise prediction for individual patients. Intermediate‑risk disease is heterogeneous: patients with a single risk factor may have outcomes closer to favorable‑risk, whereas those with two factors may approximate poor‑risk trajectories. [14], [15], [7], [3]
5. How to Use the OncoToolkit IMDC Calculator
On our platform, the IMDC calculator centers around a clean, single‑page form that presents each risk factor as a clearly worded yes/no question.
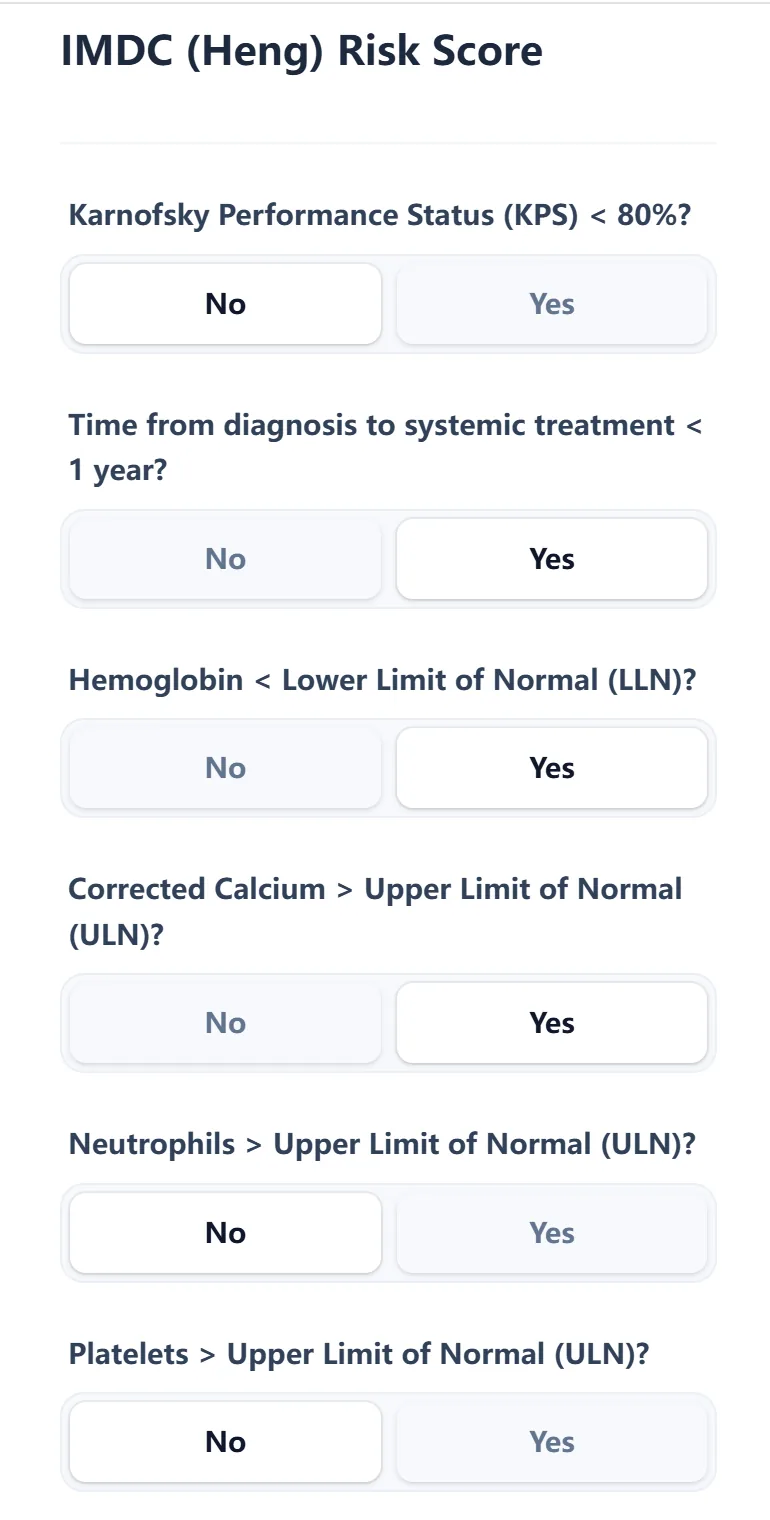
Figure 1. The input view displays all six IMDC risk factors as intuitive yes/no toggle buttons, allowing clinicians to complete the form in seconds at the point of care.
After the clinician taps “Calculate Score,” the tool instantly tallies the number of adverse factors (0–6) and maps this sum to the corresponding IMDC category using the standard thresholds.
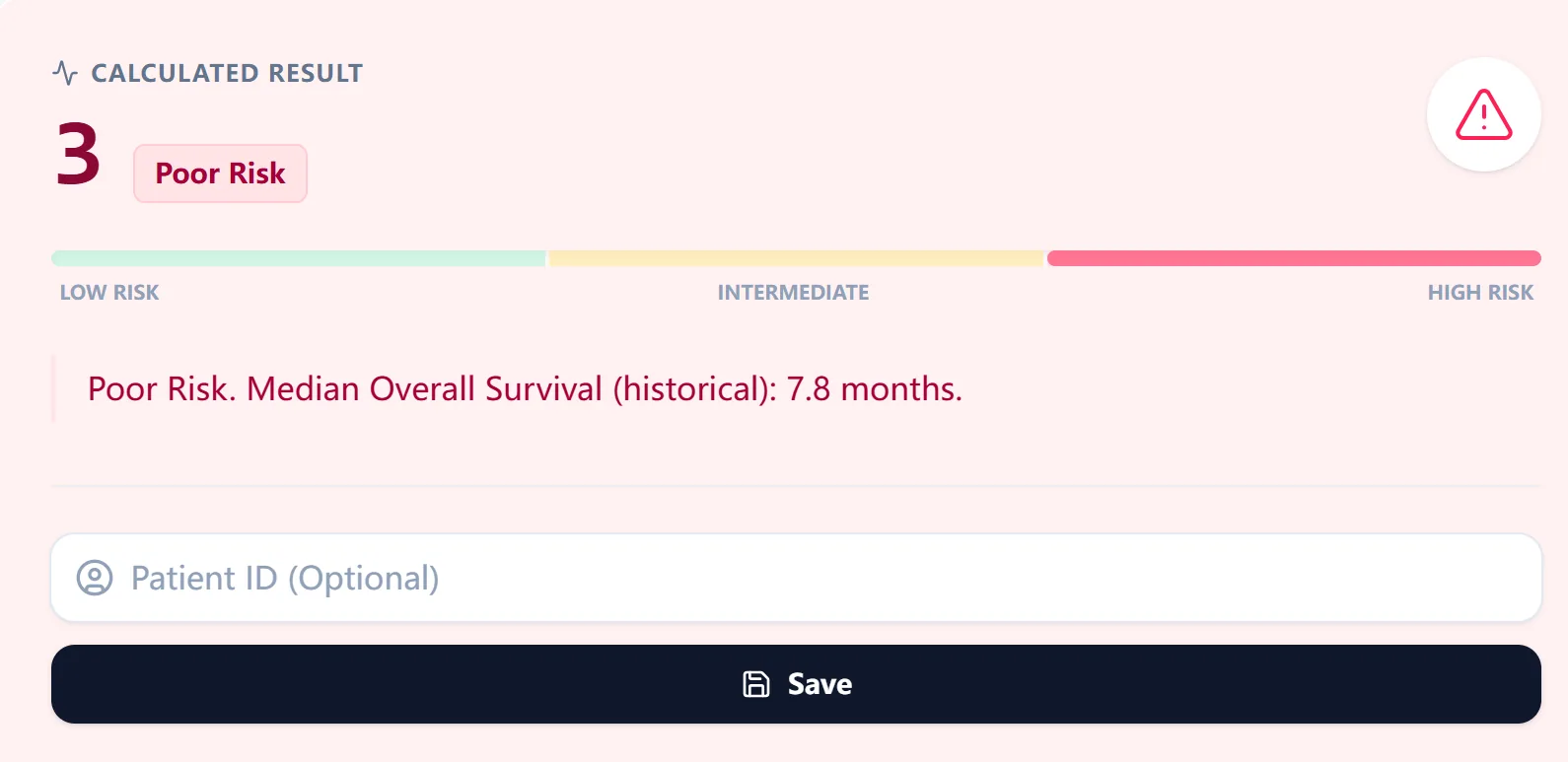
Figure 2. The result panel presents the total number of risk factors, the IMDC category, and a color‑coded survival bar with historical benchmarks.
6. Interpreting Risk Groups and Survival Benchmarks
Alongside the dynamic result, our calculator displays a concise reference table summarizing the mapping between the number of adverse factors, the IMDC group, and historical median overall survival.
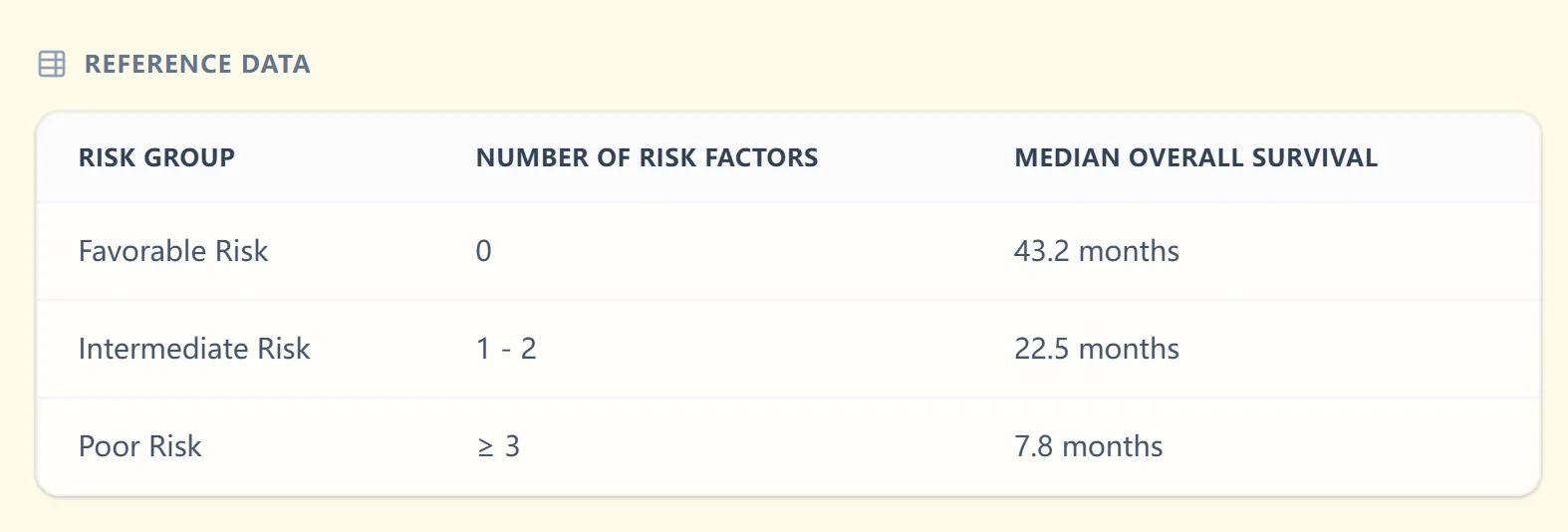
Figure 3. The embedded reference table shows how 0, 1–2, or ≥3 risk factors correspond to favorable, intermediate, or poor risk groups.
6.1 Example Clinical Scenarios
In a newly metastatic clear‑cell RCC patient with KPS 90%, hemoglobin and calcium within normal limits, and more than one year since nephrectomy, the patient yields zero risk factors (Favorable). Conversely, a patient presenting with anemia, hypercalcemia, and rapid progression within months of diagnosis is categorized as poor risk, prompting different goals of care discussions. [2], [7], [3], [1]
7. OncoToolkit: Supporting Education and Research
7.1 Routine Clinical Decision Support
Our IMDC calculator is useful at baseline staging and prior to starting each new line of systemic therapy. Because the tool is designed for one‑handed use on mobile devices, it reduces friction in busy clinics. [5], [1]
7.2 Education and Training for Oncology Fellows
The calculator doubles as a teaching tool. Trainees can adjust individual risk factors and see how the risk group shifts, building intuition for the relative impact of laboratory markers vs. performance status.
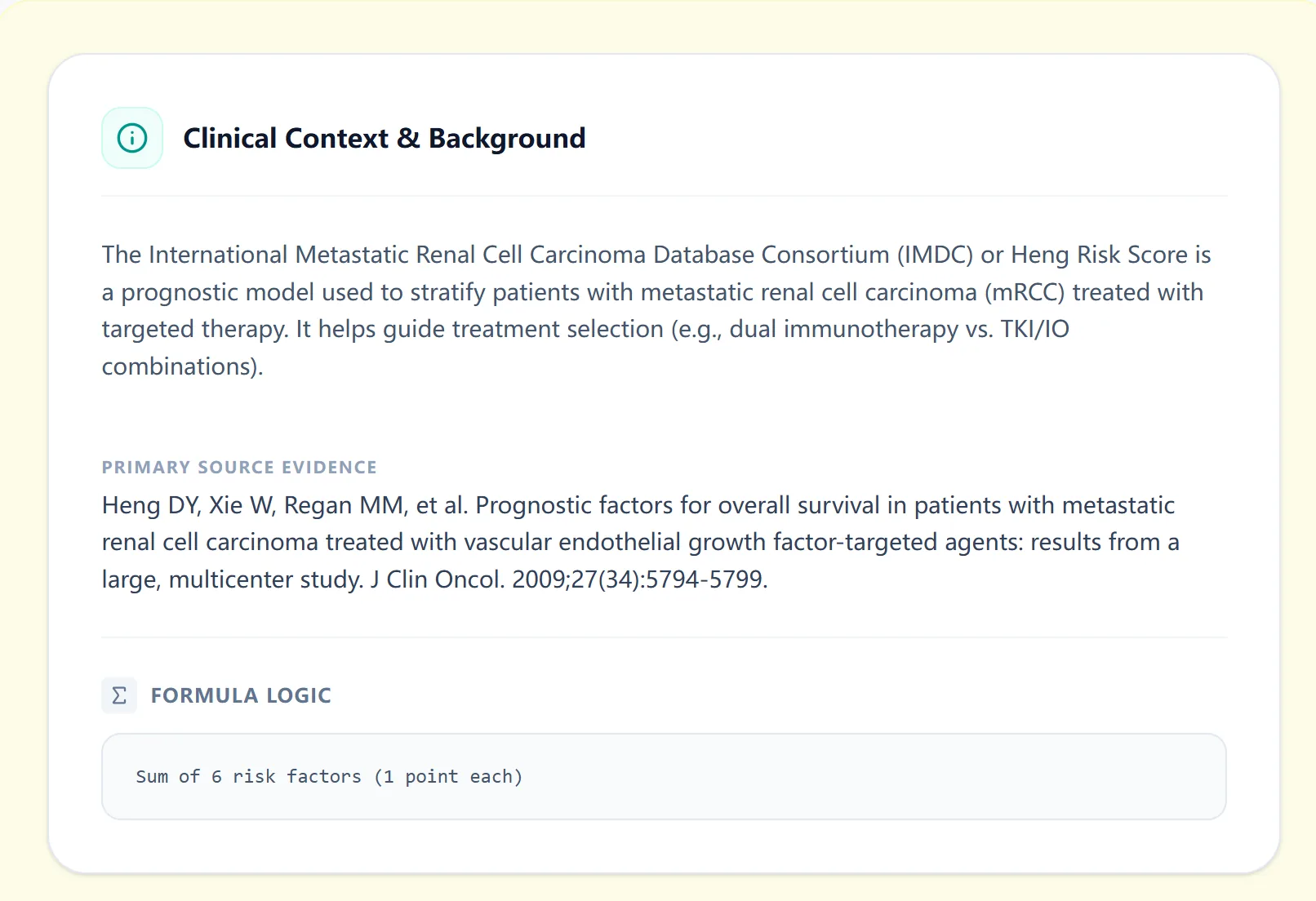
Figure 4. The background panel describes the prognostic intent of the IMDC model and links to the original publications.
7.3 Quality Improvement and Clinical Research
Standardized risk annotation enables centers to pair IMDC categories with local outcome data. This framework facilitates collaboration, ensuring that if each site uses the same calculator, survival annotations are harmonized across the institution. [13], [10], [1]
8. Clinical FAQ on IMDC Risk Stratification
How does the IMDC (Heng) Risk Score differ from the MSKCC (Motzer) criteria?
IMDC was developed in the VEGF‑TKI era and adds neutrophil and platelet counts to the MSKCC variables, providing better discrimination in modern cohorts. [8], [7]
Ready to Simplify Your mRCC Risk Assessment?
Get instant, guideline-aligned prognostic groups for your patients.
Try the IMDC Risk Score Calculator Now
Free to use. No registration required.
References
- OncoToolkit. IMDC (Heng) Risk Score Calculator. Source
- Medizin Online. Palliative systemic therapy for metastatic renal cell carcinoma. Source
- Heng DY, et al. Prognostic factors for overall survival in patients with metastatic RCC. J Clin Oncol. 2009. Source
- ACKC. International Metastatic RCC Database Consortium (IMDC) Risk Score. Source
- PMC. Implementation of clinical decision support tools. Source
- Heng JCO 2009 publication. Source
- PMC. Prognostic models in metastatic renal cell carcinoma. Source
- Motzer RJ, et al. MSKCC prognostic factors. J Clin Oncol. 2008. Source
- PubMed. Shared decision making in RCC. Source
- PMC. Validation of IMDC in targeted therapy era. Source
- Heng DY, et al. External validation of IMDC. Lancet Oncol. 2013. Source
- Renal and Urology News. Intermediate risk heterogeneity. Source
- ASCO. Survival outcomes in mRCC. Source
- Nature. Limitations of prognostic scores in RCC. Source
- OncoToolkit Clinical Asset. Result Panel.
- OncoToolkit Clinical Asset. Reference Table.
- ScienceDirect. Survival benchmarks in modern era. Source
- OncoToolkit Clinical Asset. Background Panel.
- OncoToolkit Clinical Asset. Input Form.
- ScienceDirect. Global application of IMDC. Source